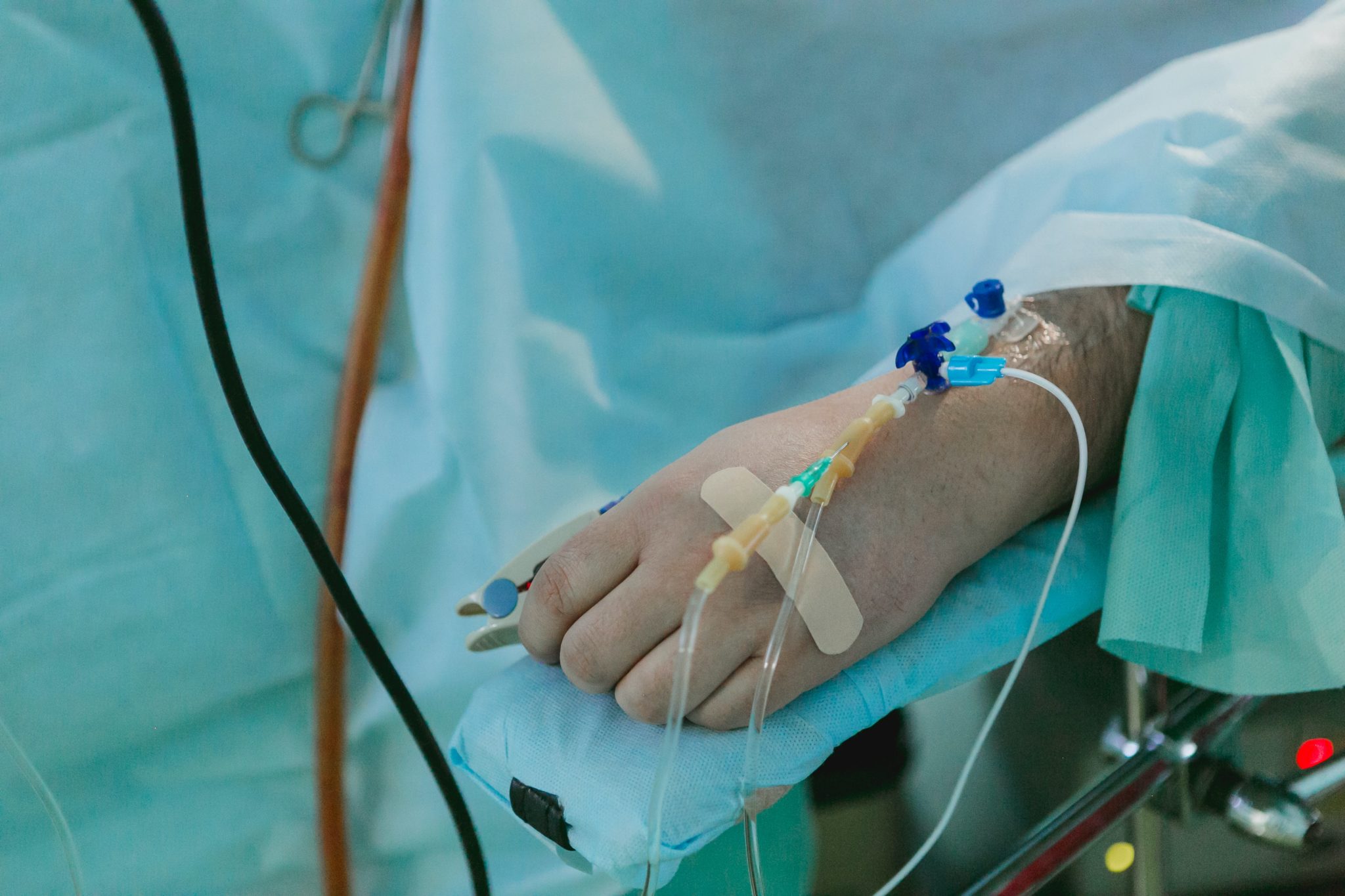
Whether you are in hospital for minor or major surgery it is almost certain you will need a catheter inserted, usually in your forearm, so fluids or medicine can be delivered.
Worldwide, catheters are the most commonly used invasive medical device.
In fact, up to 90% of hospital inpatients need one, but despite that very high rate of use a huge percentage of catheters become blocked and fail.
The experience of having a catheter re-inserted because it has become blocked is an all too common uncomfortable patient event.
For babies and children, it can also be distressing and for health systems it’s a considerable cost. The device itself only costs a few dollars, but the time and effort to reinsert the device totals well over $60 per replacement.
A team of bioengineers at Perth’s Harry Perkins Institute of Medical Research (Perkins) worked in collaboration with interstate and international vascular experts to see if an engineering solution could overcome the problem.
Associate Professor Barry Doyle heads up Vascular Engineering and the VascLab at the Perkins, and UWA. His expertise is in calculating pressure and flow in blood vessels.
In many ways he says his work is not dissimilar to the expertise of deep- sea oil and gas engineers who analyse pressure and flow inside pipes to identify points of weakness, but his work is on a much smaller scale.
A recent study he led determined an algorithm for simulating blood flow and pressure inside the aorta. The aorta is a large artery that carries blood out of your heart and sometimes balloons or leaks blood, which can be very serious.
Assoc Prof Doyle’s algorithm helps to assist surgeons determine risk and then tailor treatment options for their patients.
In relation to catheters, the team examined the approach medical staff currently take to try and avoid blockages. One of these approaches is to keep a steady flow of saline running through the catheter.
It is technically called TKVO, which simply translates as ‘to keep the vein open’ and is where clinicians allow a trickle of saline to flow through the device when not in use to, literally, keep the vein open.
Anyone who has had an extended hospital stay will be familiar with the bags of saline hanging on stands with lines attached to your catheter.
This steady flow of saline hopefully means the catheter is still able to be used when the next dose of pain relief or other medication is to be run through the line.
However, despite widespread TKVO use, clinicians do not know what the optimum TKVO flow rate is and there are no clear clinical guidelines.
Too much risks fluid overload, too little is useless and the device blocks.
The challenge for the bioengineering team was to understand the dynamics of the fluids and why blockages might still occur, and then determine the optimum flow rate.
The team simulated saline infusion and assessed flow in two forearm veins, one larger and one smaller, using computational fluid dynamics under various venous flow rates and saline flush rates.
Based on their simulations the team has proposed a specific flow rate to keep the vein open which is effective across different venous flow rates and peripheral vein sizes.
This work is the first data that demonstrates what TKVO rates might be useful across a range of clinical scenarios that factor in different vein sizes and vein blood flow rates.
It shows why some rates work better than others.
Through their work, the team believes that flushing the catheter (forcing saline through the catheter to disrupt blockages forming) might actually be causing damage to the vein itself, which could lead to further problems. In other words, the process used to unblock the catheter might be contributing to the blockage.
The next step is to run a clinical trial testing the recommended TKVO rates on healthy volunteers before trialling it on patients.
The hope is to provide clear evidence on TKVO and compare it to the flushing procedure often used.
The Perkins work was undertaken in collaboration with Prof Sam Keogh from Queensland University of Technology, who is the former President of the Australian Vascular Access Society, as well as Dr Peter Carr from the National University of Ireland Galway and Associate Professor Andrew Bulmer from Griffith University.
All three are part of the Alliance for Vascular Access Teaching and Research (AVATAR Group) which is a world leading group who investigate all aspects of vascular access.
Collaboration with AVATAR will help this work move out of the lab and to the bedside, ultimately helping to improve how these catheters are used and, importantly improve a patient’s experience during their stay in hospital.
Related news:
- Full paper download available here.
- Published in the Journal of the Association of Vascular Access 6 July 2021 (paywall)
- Twitter post 12 July 2021 https://twitter.com/vasclab_uwa/status/1414380706550083586
- 20 September 2019 Engineers Offer New Hope for Blood Vessel Surgery
- 8 March 2018 Biomedical Engineers Investigate Why Millions of Catheters Fail

Associate Professor Barry Doyle, Joint Head of the Cardiovascular Science and Diabetes Program and Head of Vascular Engineering at the Perkins.
