
Analysis of the environment that surrounds liver cancer tumours has revealed that patients with a high concentration of a certain cell type have early return of aggressive cancer but do respond better to immunotherapy.
‘Presence of onco-fetal neighborhoods in hepatocellular carcinoma is associated with relapse and response to immunotherapy’ published in Nature Cancer.
The hunt to discover a biomarker that predicts if a patient’s liver cancer is likely to return after surgery has so far eluded researchers.
Currently the most common type of liver cancer, hepatocellular carcinoma (HCC) accounts for approximately 90% of primary liver cancers and recurs within five years in 70-80% of patients.
Five-year survival of liver cancer is only 18%. This makes it critical to identify patients at high risk of recurrence after surgery and to identify the optimal treatment options at the time of cancer diagnosis.
A team led by Dr Ankur Sharma at Perth’s Harry Perkins Institute of Medical Research has discovered that patients with a high level of a certain cell type, so called “oncofetal cells” or fetal-like cells, not only are much more likely to have an aggressive form of liver cancer return within six months but do respond well to immunotherapy.
“Even when all the cancer is surgically removed, liver cancer returns for half of all patients within two years and for some it comes back within six months,” Dr Sharma said.
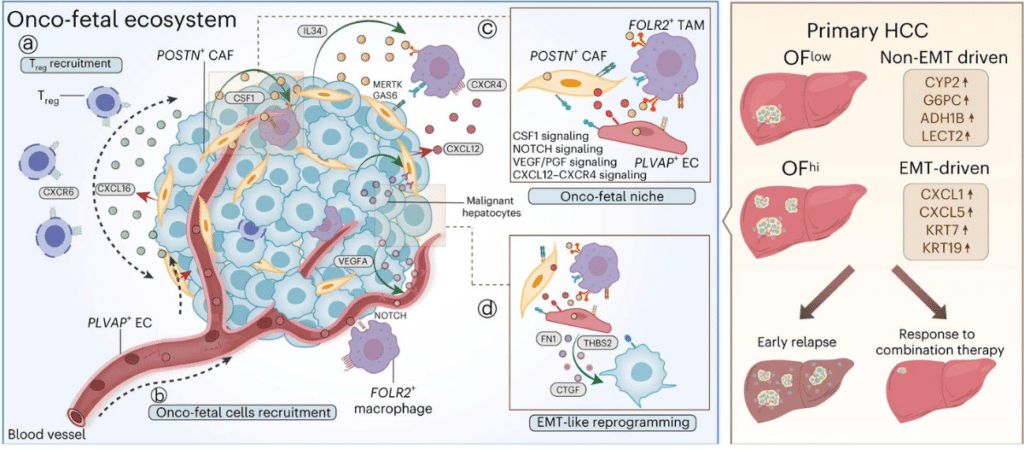 The team analysed patient samples from Sydney, Perth and Singapore and found much higher levels of fetal-like cells in the patients whose cancer returned within six months compared to those who had recurrence in two years. Oncofetal (fetal-like) cells are very adaptable and behave like embryonic (fetal) cells. They originate within the tissue surrounding tumours and provide a ‘fertile soil’ for ‘malignant seeds’. This is the reason that even after a tumour has been surgically removed, these cells remain and can lead to cancer recurrence.
The team analysed patient samples from Sydney, Perth and Singapore and found much higher levels of fetal-like cells in the patients whose cancer returned within six months compared to those who had recurrence in two years. Oncofetal (fetal-like) cells are very adaptable and behave like embryonic (fetal) cells. They originate within the tissue surrounding tumours and provide a ‘fertile soil’ for ‘malignant seeds’. This is the reason that even after a tumour has been surgically removed, these cells remain and can lead to cancer recurrence.
“By analysing the microenvironment, which surrounds and nourishes the tumour, we found some patients have high levels of fetal-like cells. Their presence predicts the likelihood of recurrence.
“We also found that patients with high levels of the fetal-like cells respond well to a newly approved immunotherapy combination of Atezolizumab plus Bevacizumab, which works by targeting blood vessels and immune cells in tumours.
“This suggests that if those patients were given immunotherapy as well as surgery at the time of diagnosis, rather than after the cancer has returned, their prognosis can be improved.
“This research not only provides a biomarker but provides a solution,” Dr Sharma said.
IMAGES: Header: Dr Sharma with the Oncofetal Ecosystem Laboratory team at the Harry Perkins Institute of Medical Research
